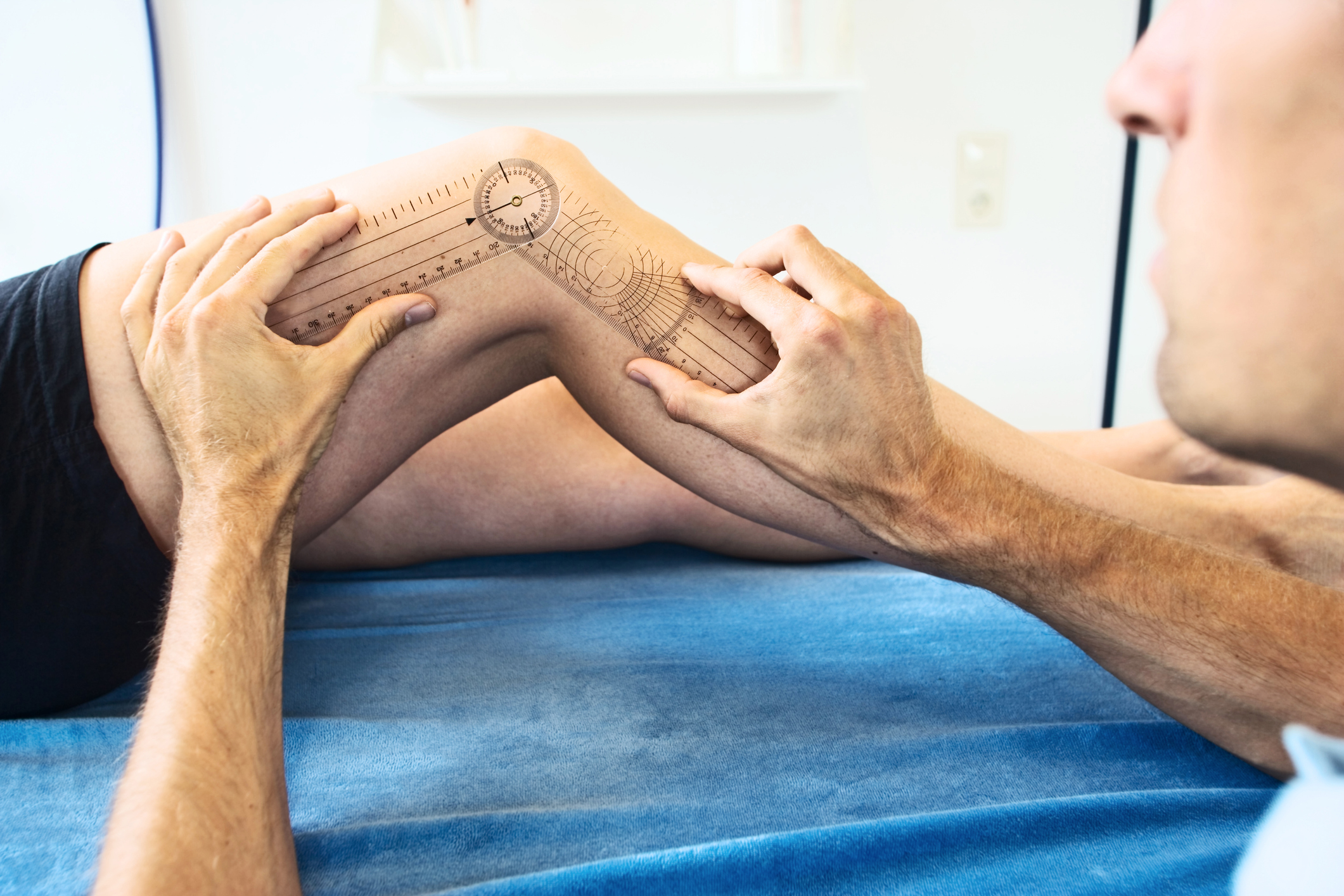
Pre Surgical Rehabilitation (Prehab)
Physical therapy is essential for patients preparing for or recovering from surgery. If you have a surgery scheduled, ask your physical therapist to prepare an exercise routine that will strengthen the muscles surrounding the joints/injured area beforehand – reducing recovery times.
Managing a patient’s BMI can also reduce pain and improve outcomes pre & post-surgically. Physical therapists can treat patients for their pain (potentially related to obesity) and can provide general population information to patients regarding healthy eating, healthy recipes, and general daily activity.
Physical therapists will also be able to provide instructions on how to prepare your home and help make sure you are as comfortable as possible during the first few days of recovery.
Post Surgical Rehabilitation
Your doctor will prescribe physical therapy after surgery. We recommend scheduling your initial visit with us prior to the date of surgery. In most cases – rehabilitation will begin at home and then will transfer to an outpatient facility such as ourselves. Post-surgical programs may include:
- Reduction of pain and swelling
- Wound care
- Improvement of strength and flexibility
- Balance and gait retraining (for lower extremities)
- Return to activity – modified duties
- Home exercise programs
- Patient education
It’s important for post-surgical patients to continue their rehabilitation program even after the pain has subsided. Getting rid of pain is one of the top priorities, but functionality, strength, and rehabilitation goals may take longer to fully achieve.
Common Post Surgical Physical Therapy Services
Total Joint Replacements
Expand For More Info
Total Knee Replacements
Typically, patients need outpatient physical therapy after therapy at home, which usually begins two to four weeks after surgery. Outpatient physical therapy is recommended for three times a week for up to three months.
Therapy goals initially are to reduce swelling and pain, and improve knee range of motion in both directions. To achieve these goals, treatment may consist of soft tissue massage to increase circulation and decrease swelling, stretching to improve flexibility, patellar mobilization, range of motion exercises, and modalities such as ice and electrical stimulation to help decrease pain and swelling.
Physical therapy will progress to lower extremity strengthening exercises, balance activities, and fine-tuning the gait pattern. Various activities and techniques will be used to improve strength, balance, and gait. As patients reach the end of their course of physical therapy, a personalized home exercise program is developed with the focus on independence with all ADL’s and returning to activities such as walking, swimming, dancing, golf, and biking. It is important for patients to stay active and maintain strength, flexibility, and endurance.
Total Hip Replacements
Postoperative physical therapy after a Total Hip Replacement is essential to recovery. Your physical therapist will follow your physician’s protocol and will focus on range of motion exercises, progressive strengthening exercises, gait training, balance training, and activity-specific training to meet your specific needs. Modalities such as ice and e-stim may be used to help reduce discomfort and swelling. It is very important to complete your home exercise program as directed by your physical therapist and physician. Treatment typical includes:
- Range of motion exercises
- Strengthening exercises
- Balance training
- Gait training
- Activity specific training

Post Surgical ACL Tear Recovery
Expand For More Info
The knee is essentially a hinged joint that is held together by four ligaments. They include the medial collateral (MCL), lateral collateral (LCL), anterior cruciate (ACL), and posterior cruciate (PCL) ligaments. The ACL runs diagonally in the middle of the knee, preventing the lower leg from sliding out in front of the thigh, as well as providing rotational control to the knee.
How Long Does it Take to Recover from ACL Surgery?
Recovery times will differ depending upon the severity of the tear, but by 16-22 weeks most patients reach full Active Range of Motion (AROM) and are focused mostly on strengthening. Below is a tentative schedule of what you can expect:
- Week One:
- Decrease Pain and Effusion
- Full Passive Knee Extension
- Weeks 2-4: Keep Full Extension
- Weeks 4-10: Achieve Full Range of Motion
- Weeks 10-16:
- Work to normalize strength
- Increase power along with endurance
- Increase neuromuscular control
- Progress functional training
- Weeks 16-22:
- Full active and passive range of motion
- Proprioception at 100%
- Functional tests at 90%
- Strength at 85%
Post ACL Return to Sport
An ACL injury can leave a player out of the game for a while. Physical therapy is needed to help rebuild knee strength. Return to sports programs will include mobility and strength exercises such as knee flexion and extension, heel slides, and isometric quadriceps exercises. As the knee joint gets stronger, plyometric drills will be introduced to the therapy to see whether the knee is strong enough to play competitive sport. These exercises may include resistance band jumps, hopping exercises, and box jumps.
Post Surgical Rotator Cuff Recovery
Expand For More Info
A patient will typically be referred for rotator cuff surgery when 90% or more of the tendon is torn. The most common causes of rotator cuff injuries are aging, overuse of overhead activities, and heavy lifting.
Surgery should never be taken lightly, so we wanted to take some time to inform you about what to bring before surgery, things that can help you immediately after, and then give an idea of what to expect as you go through a post-surgical rotator cuff physical therapy treatment plan. These are general guidelines. More specific expectations can be given by your healthcare provider.
5 Stages of Rotator Cuff Tear Recovery
Post-surgical rotator cuff physical therapy care can vary based on the patient’s needs and ability levels. Depending upon the severity of the tear, physical therapy can work with patients to heal the tendon and reduce pain.
Stage 1: Immobilization
This period may last 4-6 weeks and may be intermittent with the therapist being able to do slight motions to the arm to keep the joint from getting stiff.
Stage 2: Passive motion
At first, the therapist will provide the muscle to move the arm, but over time, you’ll be educated in the use of pulleys, stretch straps and table stretches to allow the joint to move while keeping the muscles fully relaxed.
Stage 3: Active-Assisted motion
Self-ranging exercises will use the uninvolved arm to move the involved arm. The surgical arm’s responsibility will slowly increase up to 100% of the weight of the arm. Then, you’ll be ready for active motion
Stage 4: Active motion
The active motion phase begins when the arm is able to carry its own weight against gravity but is not yet ready to lift, push or pull objects. Once you can achieve the full expected active range of motion against the weight of gravity, and with your physician’s approval, you’ll be ready to add weight.
Stage 5: Strengthening
Your therapist will recommend exercises that you can do at home in order to improve the arm’s tolerance for strength and to reduce the strain on the arm when you come into therapy.