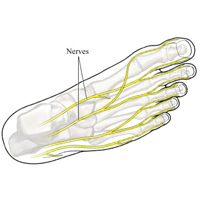
Diabetic neuropathy is a type of nerve damage associated with diabetes. It results in damage to the nerves in a person’s feet, legs, and eyes, and to the nerves that control bodily functions, such as digestion, blood pressure, and heart rate. Diabetic neuropathy can lead to serious complications, including ulcers, infection, and limb loss.
Causes
Researchers believe that diabetic neuropathy is likely caused by a combination of factors, including:
• Metabolic problems (e.g., high blood glucose)
• Damage to blood vessels
• Autoimmune factors
• Genetics
Risk Factors
The following factors are thought to increase the risk of diabetic neuropathy:
• Older age
• Having diabetes for 25 years or more
• Having type 2 diabetes
• High blood pressure
• Lifestyle factors (e.g., smoking, alcohol use)
• Obesity
• Lack of exercise
• Peripheral vascular disease
• High cholesterol
Symptoms
• Symptoms of diabetic neuropathy may include:
• Numbness in the extremities
• Tingling in the extremities
• Pain in the extremities
• Wasting of the muscles of the feet or hands
• Indigestion
• Nausea or vomiting
• Diarrhea or constipation
• Dizziness or fainting
• Urination problems
• Impotence or vaginal dryness
• Weakness in arms and/or legs
• Foot drop
• Muscle cramps
• Weakness of facial muscles resulting in drooping eyelid, drooping mouth, facial droop, difficulty swallowing
• A prolonged feeling of fullness after eating, and/or abdominal pain
• Heat intolerance due to a decreased ability to sweat normally
If you have diabetic neuropathy, you are at increased risk for developing other types of neuropathies, such as carpal tunnel syndrome.
Diagnosis
Your doctor will ask about your symptoms and medical history. They will also do a physical exam. Other tests may include:
• Foot exam — to assess sensation in the foot
• Nerve conduction studies — to test nerve activity
• Electromyography — to determine how muscles respond to nerve signals
• Quantitative sensory testing — the use of stimuli (e.g., vibration) to check for neuropathy
• Quantitative sudomotor axon reflex test — a test to evaluate the nerve supply of sweat glands
• Heart rate tests — to determine how the heart responds to changes
• Ultrasound — to view internal organs
• Biopsy — to remove a sample of nerve or skin tissue for examination
Treatment
Talk with your doctor about the best treatment plan for you. Your overall treatment plan may include:
• Blood glucose management
• Foot care regimen
• Transcutaneous electrical stimulation (TENS)
• Physical therapy
Diabetic neuropathy can be very painful, so the thought of physical therapy may not seem appealing. However, physical therapy will help you regain motions that you may have lost or improve your balance when walking. The goal of treatment for diabetic neuropathy is maintaining and improving your range of motion, as well as strengthening your muscles. Simply learning how to stand from a sitting position without getting dizzy may be a part of your physical therapy treatment. Other exercises may include gait training and maneuvering over various surfaces to avoid tripping or falling and to improve overall balance when you go about your everyday activities. Regaining sensation in the hands and feet can also be treated with various exercises during physical therapy.
Prevention
The best way to prevent diabetic neuropathy is to regularly monitor and manage your blood glucose levels. Your doctor can instruct you about how often to check your levels and what the numbers mean.
This content was created using EBSCO’s Health Library references provided online