Shoulder pain can sneak up on you from sports, work, or everyday activities like lifting, reaching, or even sleeping in a bad position. A common cause of this type of pain is a rotator cuff injury. Physical therapy is one of the most effective ways to treat it, often without even having to go through surgery.
How Physical Therapy Helps Rotator Cuff Injuries
Physical therapy offers a proven, non-invasive path to recovery, helping you regain strength and reduce pain. It also focuses on improving mobility and flexibility through guided stretching and range-of-motion exercises, easing stiffness that can worsen pain. To manage discomfort, therapists use manual techniques, activity modifications, and targeted exercises to reduce inflammation without relying solely on medication.
One of the biggest misconceptions is that surgery is always required for a rotator cuff tear, although many people recover successfully with physical therapy alone. If surgery is necessary, your doctor can refer you to a physical therapist for a post-surgical rotator cuff tear treatment plan.
If your shoulder has been bothering you, it’s worth getting it checked. Physical therapy focuses on treating the root cause, not just the pain. Because no two injuries are the same, each treatment plan is personalized based on your strength, mobility, and daily activities. Schedule an appointment with a physical therapist today.
Not sure if you have a rotator cuff injury? Here’s what you need to know:
What Is a Rotator Cuff Injury?
Your rotator cuff is made up of four muscles and their tendons that stabilize your shoulder and allow you to lift and rotate your arm in many directions. Because the shoulder has such a wide range of motion, it is also more vulnerable to injury.
Rotator cuff injuries include:
- Tendonitis (inflammation)
- Partial or full tears
- Strains from overuse
- Impingement (pinching of the tendons)
Rotator Cuff injuries often develop gradually from repetitive overhead movements like throwing, swimming, or lifting, or from wear and tear over time.
Common Symptoms of Rotator Cuff Injuries:
Many people notice subtle warning signs first, such as:
- Shoulder pain when lifting or reaching overhead
- Weakness in the arm
- Limited range of motion
- Clicking or popping sensations
- Pain at night, especially when lying on the affected shoulder
Ignoring these symptoms can worsen the pain over time, making early treatment important.
How to Prevent Future Shoulder Injuries
Consistent conditioning and awareness go a long way in protecting your shoulders. Here are a few ways you can reduce your risk by:
- Strengthening shoulder and upper back muscles
- Avoiding repetitive overhead strain when possible
- Taking breaks during repetitive tasks
- Maintaining good posture
- Warming up before physical activity
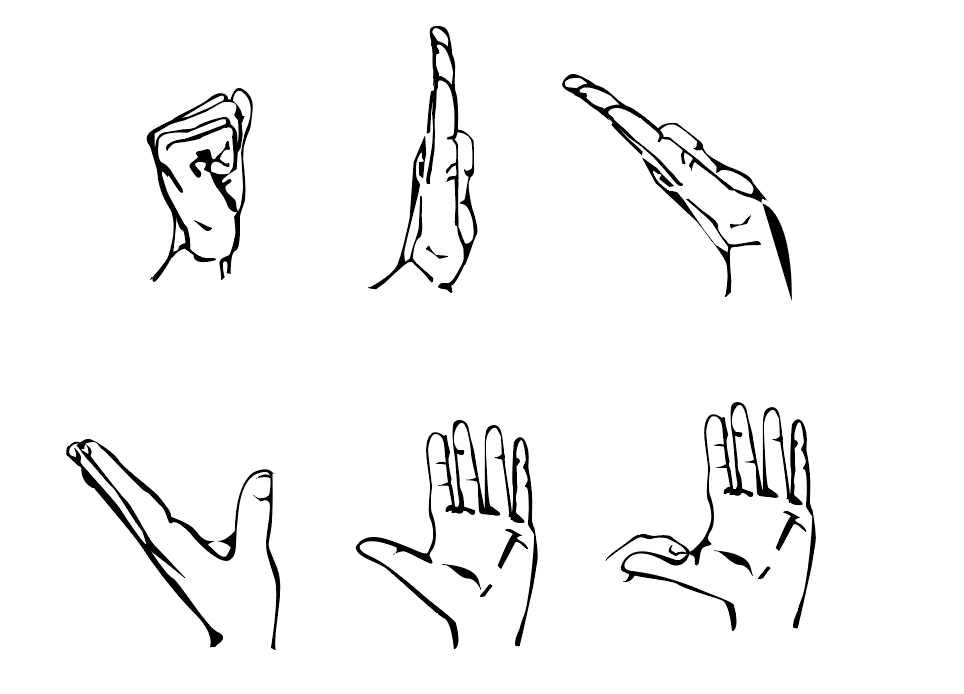
Here are some exercises that can help get lessen mild shoulder pain and prevent an injury from occurring.