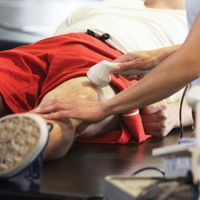
Every treatment is truly a modality with exercise (including Therapeutic Exercise, Therapeutic Activities and Neuromuscular Re-education) being the most popular and effective.
ULTRASOUND: Can be performed for thermal or non-thermal benefits. A crystal in the sound head vibrates at a specific frequency (usually 1 or 3 MHz) when an electrical current is passed through the crystal. The ultrasound waves that are produced are absorbed best by high collagen content tissues (tendon, ligament, and muscle). The frequency controls the depth of penetration with 3 MHz being more superficial and heating up more quickly than 1 MHz. An effective treatment area is no greater than twice the area of the ultrasound head (5cm^2 US head). Physical therapists use ultrasound frequently on tendinosus injuries, or plantar fasciitis as well as ligament injuries, and in conjunction with transverse friction massage and exercise.
ELECTRICAL STIMULATION: Most often performed in outpatient orthopedic PT clinics for muscle re-education or pain control. The waveform, frequency and wavelength are different depending on the reason for using this modality.
With neuromuscular estim (NMES) two electrodes are typically used. Physical therapists use NMES to the quadriceps (specifically VMO) to regain quadriceps control to restore active terminal knee extension. There is an on and off time with NMES, and the patient is usually performing a quadriceps exercise during the time the NMES is on.
When electrical stimulation is used for pain control the term TENS is commonly used, which stands for Transcutaneous Electrical Nerve Stimulation, but even NMES is technically TENS. With TENS various set-ups can be used, but the most common is IFC (Interferential Current) at 80-150 Hz with 40% scan. This requires 4 electrodes in a crossed-diagonal pattern with the treatment area in the middle. An interference pattern is created, and varies throughout the treatment giving the sensation that the current is moving around, and preventing the patient from becoming too accustomed to the sensation. There can be some carryover of pain-relieving TENS effects between sessions, but I generally consider this to have a temporary effect lasting for up to 2-3 hours after the session. Often heat or ice is applied during the treatment as well. If you want to prescribe a home TENS unit for a patient for pain management we are happy to assist by working with vendors to obtain a device for a patient, and to teach them how to use the device.
TRACTION: Static (constant tension) traction is most commonly used, unless the patient’s condition is very reactive, and then intermittent traction may be used. A home traction unit may also be ordered for a patient, and we can train the patient in the set-up and usage of those devices. They are available for both cervical and lumbar traction, but lumbar traction is much less commonly used. A patient must be able to tolerate 20# of cervical traction, typically, for insurance to cover a home device.
PHONOPHORESIS AND IONTOPHORESIS: Both of these are drug delivery methods. Iontophoresis uses direct current electricity to drive a charged medication deeper into the tissues while phonophoresis is the usage of a medication in an ultrasound gel or cream. The research support is better for iontophoresis than phonophoresis, but neither are very good. Iontophoresis most often is done with dexamethasone with a negative polarity and the medication is placed under the negative electrode. With phonophoresis the US, at least theoretically, opens up channels to allow the medication to be absorbed more readily, but in doing US with a medication, the ultrasound transmission is not as good as with the normal ultrasound gel.
WHIRLPOOL: Cold or warm whirlpools are somewhat common still in athletic training rooms, but not utilized nearly as much in a PT clinic. They also used to be used very commonly for wound debridement, but the time and expense of the water and sterilizing the whirlpool after use, coupled with the existence of good medicinal/chemical methods for wound care have made whirlpool use for that purpose much less common.