Shoulder Pain Physical Therapy Can Fix
Carrying the weight of the world on your shoulders? When everything rests on your shoulders, they’re more prone to injury. Constantly carrying your children, overtraining, too much lifting, or throwing your heavy backpack over your shoulders every morning can lead to a painful injury. If you already have pain or difficulty with your shoulders, physical therapy is the way to go.
Whether it’s rotator cuff tears or other injuries to the muscles surrounding the shoulder, physical therapy for shoulder pain is often a successful, non-surgical treatment. It aims to strengthen the muscles around your shoulder to heal and improve its function and your mobility.
Common Causes of Shoulder Pain
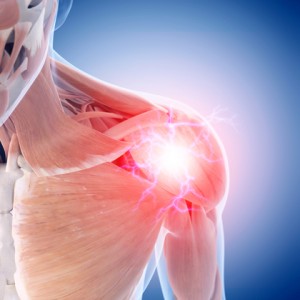
Not all shoulder pain is created equally! It is not all caused by the same thing. The anatomy of a shoulder is a bit complex, consisting of many different parts. The shoulder is a ball and socket joint made up of the humerus (arm bone), the scapula (shoulder blade), and the clavicle (collar bone). There are many ligaments that support the shoulder, and many muscles are attached to help you move in many different directions. This leads to many potential causes of the pain you may be experiencing and here are the most common causes of shoulder pain.
Tendonitis
Tendinitis is a very common condition that often sends people straight to a physical therapist for pain relief. A tendon is a cord that connects muscle to bone. Most tendinitis is a result of inflammation of the tendon and usually affects people who take part in many physical activities, or work at a job that requires them to use lots of repetitive motions every day.
The most commonly affected tendons in the shoulder are the four rotator cuff tendons and one of the biceps tendons. The rotator cuff is made up of four small muscles and their tendons that cover the head of your upper arm bone and keep it in the shoulder socket. Your rotator cuff helps provide shoulder motion and stability. If you make the same repetitive motions every day to play your sport or do your job, such as an athlete who plays tennis or a professional painter, you could be at high risk for developing tendonitis in your shoulder. Those who are at high risk for developing this condition should be aware of how important it is to not only visit a physical therapist regularly but also rest their shoulders often to prevent chronic pain.
Tendon Tears
Splitting and tearing of tendons may result from an acute injury or degenerative changes in the tendons due to advancing age, long-term overuse, wear and tear, or a sudden injury. These tears may be partial or may completely separate the tendon from its attachment to bone. In most cases of complete tears, the tendon is pulled away from its attachment to the bone. Rotator cuff and bicep tendon injuries are among the most common of these injuries.
If you experience a partial or full tendon tear, the pain can be searing and require regular appointments with a physical therapist -but there’s good news! In a 2013 study, up to 75% of people with a full tear in their rotator cuff were able to rehab their shoulder without the need for surgery (Kuhn et al. Shoulder and Elbow, 2013 October).
Instability
Shoulder instability occurs when the head of the upper arm bone is forced out of the shoulder socket. This can happen as a result of a sudden injury or from overuse. Shoulder dislocations can be partial, with the ball of the upper arm coming just partially out of the socket. This is called a subluxation. A complete dislocation means the ball comes all the way out of the socket. Once the ligaments, tendons, and muscles around the shoulder become loose or torn, dislocations can occur repeatedly. Recurring dislocations, which may be partial or complete, cause pain and unsteadiness when you raise your arm or move it away from your body. Repeated episodes of subluxations or dislocations lead to an increased risk of developing arthritis in the joint.
Non-surgical physical therapy treatment for instability will typically focus on reducing the strain at the shoulder in a downward or backward position during functional task performance. The therapist will likely present a number of restricted motions and ways to perform functional daily tasks without putting strain on the ligaments. In the case of a painful shoulder, the therapist will recommend anti-inflammatory techniques and positions of the shoulder at night and during sustained or repetitive task performance.
Arthritis
Often people will avoid shoulder movements in an attempt to lessen arthritis pain. This sometimes leads to a tightening or stiffening of the soft tissue parts of the joint, resulting in a painful restriction of motion. Two common forms of shoulder arthritis without a previous injury involve osteoarthritis and rheumatoid arthritis.
Osteoarthritis
This “wear and tear” condition involves the smooth cartilage that covers the ends of the bones where they form a joint. This cartilage allows the bones to move against each other smoothly. When you have osteoarthritis, your cartilage wears away, causing your bones to rub against each other.
When working with patients that suffer from Osteoarthritis, physical therapists focus on maximizing the amount of safe motion that the shoulder can perform and provide education on how to alter your activities to stay within that motion. Patients are likely to be provided with a home exercise program that includes strengthening the uninvolved muscle groups in order to provide support for those that are inflamed or damaged.
Rheumatoid arthritis (RA)
Rheumatoid arthritis impacts the joint lining, or synovium, that lubricates the joint so it can move easier. Unlike osteoarthritis, RA is an autoimmune disorder. This means the body attacks itself, and in this case, it attacks the synovium. It usually affects multiple joints, typically on both sides of the body, such as both shoulders.
Bursitis
The shoulder is made up of a very complex network of moving parts. One of the main components that make up the shoulder is called the “bursa.” Bursae are small, fluid-filled sacs that are located in joints throughout the body, including the shoulder. They act as cushions between bones and the overlying soft tissues to help reduce friction between the gliding muscles and the bone.
Sometimes, excessive use of the shoulder leads to inflammation and swelling of the bursa between the rotator cuff and part of the shoulder blade and can become painful. Many daily activities, such as combing your hair or getting dressed may become difficult.
Impingement
Shoulder impingement can occur when the top part of the shoulder blade puts excessive pressure on the underlying soft tissues in the arm when it is lifted away from the body. As the arm is lifted, the shoulder blade rubs, or “impinges” on, the rotator cuff tendons and bursa. This can lead to bursitis and tendinitis, causing pain and limiting movement. Shoulder impingement is a condition that occurs when the top part of the shoulder blade lifts away from the body and puts too much pressure on the underlying soft tissues in the arm. As the arm lifts, the shoulder blade rubs against the bursa and tendons. If this condition goes untreated, an impingement in the shoulder can result in bursitis and/or tendinitis.
Not all shoulders are created equal, so an individualized plan for physical therapy treatment needs to be designed and instructed. Many times, there needs to be a certain amount of manual stretching and joint mobilizations provided by a trained and licensed Physical Therapist as well. The vast majority of people who suffer from shoulder impingement are treated successfully with these steps of rest, medications, stretching exercises, and the temporary avoidance of overhead reaching. If symptoms persist or if there is significant weakness present that is not improving the rotator cuff may be damaged and require further assessment from an Orthopedic MD.
Fracture
Fractures are broken bones. Shoulder fractures commonly involve the clavicle (collarbone), humerus (upper arm bone), and scapula (shoulder blade). Shoulder fractures in older patients are often the result of a fall from a standing height. In younger patients, shoulder fractures are often caused by a high-energy injury, such as a motor vehicle accident or contact sports injury. Fractures often cause severe pain, swelling, and bruising on the shoulder.
Frozen Shoulder
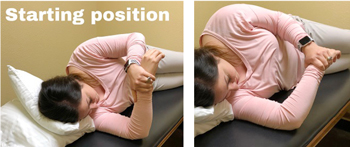
Adhesive capsulitis, also known as frozen shoulder, is a condition that occurs following an injury or alongside another shoulder condition. This is when the shoulder capsule thickens and becomes stiff and tight causing thick bands of tissue, called adhesions, to develop. If left untreated, frozen shoulder can take up to 2 years to go away on its own. Most physical therapists recommend that patients with frozen shoulders rest often in between physical therapy appointments to avoid developing scar tissue in the shoulder. On the chance that scar tissue does develop, the muscles surrounding the shoulder may eventually freeze up as well. This will limit your full range of motion and result in chronic pain.
Physical therapists are specialists and experts in evaluating, treating, and managing patients with an array of shoulder pain problems. If any of these conditions sound familiar, your therapist will examine your strength and range of motion, check your functional abilities (like reaching up and behind your back), and then come up with a personalized treatment plan to relieve your shoulder pain and restore your mobility. Don’t shrug it off and have a physical therapist guide you through your shoulder rehab today.